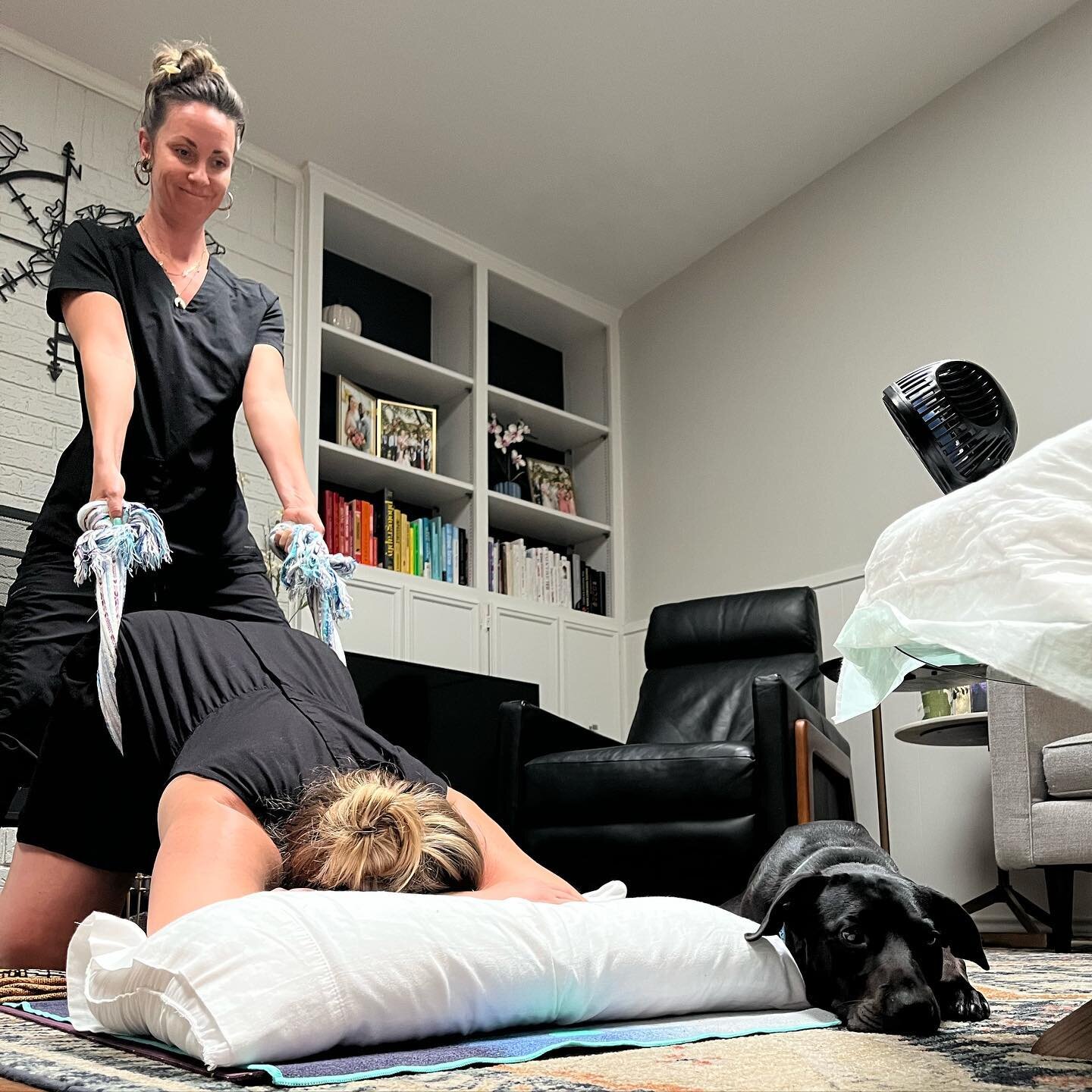
I’ve written a few posts now about pelvic floor diagnoses and about signs that you may have problems with your pelvic floor muscles. So maybe you’ve been reading and you think “Oh crap, I’ve done that!” or “OMG maybe I have that?!” And now you’re thinking… “Okay so what do I do now?”
First off, let me say the realization that what you are experiencing is not normal is a shock. I say this from personal experience. Take the time to process this. Some people may react to this realization by sticking their head in the sand. Perhaps you’ve known for a while that there is something “going on” but you aren’t sure where to start by getting treatment… or what treatment even means.
If you know that you have a problem, you are one step closer to figuring out what "it" is and towards getting treatment. Here is a list of what you may expect during your path to diagnosis and treatment.
#1 You will probably see many healthcare providers
It makes me sad to say that very few healthcare professionals get in depth training about pelvic floor problems. In physical therapy school all I had was a 3 hour lecture - that's it! I had to pursue opportunities to observe other pelvic floor professionals and to take continuing education courses after graduating to learn more.
In our hypersexual society, we have a TON of myths and misinformation floating out there about what is normal, what deserves further investigation, and possible treatment options. Providers are people too - if they didn't have any training then they may believe some of these myths! In a 2007 study of 167 physicians, over 85% stated that they received little training and were confused by the medical terminology of a chronic pelvic pain condition known as vulvodynia. This is why you may be referred to a couple different providers before you get a diagnosis. You may also have to undergo many different tests to receive a diagnosis.
You may encounter doctors or other healthcare providers who do not understand the problems you are having. While I hope this changes ASAP, in the meantime, do not give up! There are amazing practitioners out there who have spent countless hours learning and treating patients, who can help you to make a positive change in your life.
#2 You're going to have to be your own advocate
I cannot emphasize this point enough. If you take nothing away from this post, heck even this blog, then I want you to remember this:
YOU are responsible for making sure that you get the best care.
If you find that Dr. Suzie Pelvis isn't listening to a word you say or doesn't care about your values, then switch doctors. If a provider offers you different treatment options, then ask questions about them and take the time to figure out what you prefer. If you do not understand what a diagnosis/treatment/test/medication/procedure is then ASK.
Pelvic floor diagnoses require additional training and education in order to provide you the best care. Ask your providers how many patients with similar problems they have treated. Ask about their outcomes - do patients with your condition get better, worse, or stop coming? What treatments have helped in the past? How long do they spend with each patient?
Remember, the only reason that doctors, technicians, nurses, therapists, etc have a job is to take care of the patient (i.e. YOU). It is not okay for a provider to belittle you or your problems, or act as if you are lucky to get their time of day. With that being said, please keep in mind that we providers also have other patients too. You can do your part by being on time for appointments, calling in advance to cancel (when possible), being honest with your provider, and showing him or her respect.
Being your own advocate also means that you have to take responsibility for your actions. For example, if your therapist taught you a certain stretch which helps to relieve your pain but you stop stretching and your pain increases then you need to start again!
#3 You want a team
This builds and expands on point number 1. By the time you are going to get treatment, you should have a diagnosis. The best care is often going to involve a team of providers, who communicate about your case and coordinate your care. Your team may include specialists, a pelvic floor physical therapist, nutritionist, and a mental health provider. This is by no means a full list of providers. It may also help you to join a support group to speak with other people who are having an experience similar to your own.
Each of these providers brings something different to the table and with pelvic floor problems, you want a big table! This is especially important if you have other medical problems such as heart disease, neurological problems, diabetes, etc.
Emotionally, living with a pelvic floor dysfunction or diagnosis can be extremely difficult because it’s an “invisible disorder.” You can’t show people a cast and you may not even know exactly how the problem started. Pelvic floor problems are also very intimately tied to things we often don’t talk about, like leaking pee/poop, difficulty pooping, painful sex, or constant pelvic pain. Especially in the case of long term problems, it’s important to address this emotional side of pain as well. Depression, anxiety, and stress can often worsen the problems you are having and make it easier for you to experience pain. Working with a psychiatrist or counselor may be an important part of your treatment.
#3 Don’t expect instantaneous results
Treatment for pelvic floor problems are usually a marathon, not a sprint. In most cases it took a long time, maybe even years for your problems to develop/escalate to the point they are at now. It will take time to improve them as well! Also, many treatments involve lifestyle changes which take time to implement. Some of these changes include adding regular physical activity, losing weight, and retraining your internal organs and pelvic floor muscles. Give the treatments a couple months to kick in before you decide that they are not working for you.
Again, let me shamelessly promote giving pelvic floor physical therapy (PFPT) a try. There is more and more research coming out which says that PFPT should be the first line treatment for problems such as urinary incontinence (leaking pee), pelvic organ prolapse (bladder, vagina, or rectum falling out of your body), and chronic pelvic pain. Even in cases where the underlying problem is not in the muscles or tendons, PFPT can help you to manage or decrease other symptoms. For example, women with endometriosis can have tightness, tenderness, or spasms in their pelvic floor muscles as a response to the high pain levels they feel. PFPT can help to decrease these spasms and teach you more pain management techniques.
I also strongly believe that surgery should be a last resort, not a first choice treatment. If you think about it, physical therapy has fewer side effects than other treatments. Under the care of a properly trained pelvic floor therapist you may be more sore or have only a little/temporary improvement after treatment, but that’s about it. Medications usually have side effects, some of which can be worse than the original reason you started taking the medication for. Surgery carries its own risks and like any treatment, has no guarantee that it will work. Some insurances even require that you try other treatments before they will cover surgery.
So that's a few of the things you can expect. I sincerely hope that in the future anyone with pelvic problems can go to 1, maybe 2 doctors, get the right diagnosis, and get ultra-effective treatment ASAP. For now we need to spread the information to friends, family, and other healthcare providers.